What we know so far about St Andrew's Hospital failings
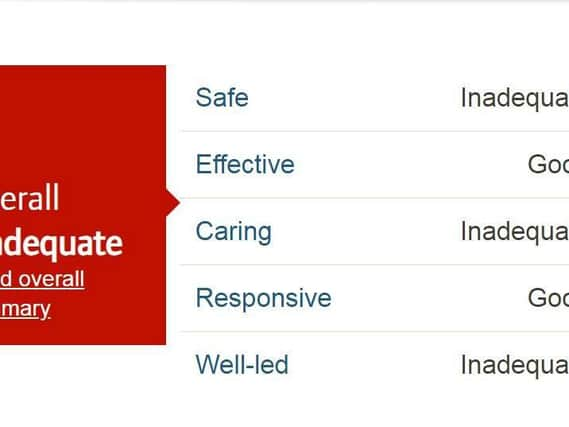

Here's what we know about the hospital and what the CQC found so concerning:
St Andrew's Healthcare - the overall charitable company - gets almost 98 per cent of its funding via NHS referrals.
Advertisement
Hide AdAdvertisement
Hide AdSt Andrew’s Healthcare Adolescents service is based in Fitzroy House, a purpose-built hospital, opened in January 2017
The building offers sensory rooms, music and arts rooms, a sports hall, gardening areas and outside space (courtyards).
St Andrew’s Healthcare Adolescents service has 11 wards and is registered to accommodate 99 patients. There were 77 patients at the service during the latest inspection. The hospital has halted all new admissions to the unit while it works out how to respond.
The inspectors found staff did not always treat patients with kindness, dignity compassion and respect. Eleven of the 15 seclusion rooms did not include furnishings such as a bed, pillow, mattress or blanket. They reviewed 13 episodes of seclusion where staff had not provided the patient with a mattress or chair. Observation records for nine episodes of seclusion detailed 28 entries describing the patient sitting or lying on the floor.
Advertisement
Hide AdAdvertisement
Hide AdStaff, on one occasion, did not respect a patient’s privacy and dignity when changing the patient’s clothing and did not ensure that female staff assisted with this for female patients. It was the inspection team’s view that this practice was uncaring, undignified and disrespectful.
Managers had not ensured that they consistently identified or addressed safety concerns quickly enough. There were sharp edges on door frames in seclusion rooms and extra care suites, blind spots in seclusion rooms and pieces of exposed sharp metal in extra care suites. Staff did not always record, accurately, the events that took place during incidents. There was discrepancies between incident reports, staff recollection and the images captured on CCTV.
Staff did not follow best practice when using seclusion and long term segregation. This is despite the CQC raising the issue on no less than 12 separate occasions. Staff secluded three patients for longer than necessary.
Staff applied blanket restrictions without justification. All wards had imposed set snack times for patients. Other restrictions included access to drinks and takeaways, patients not allowed to wear shoes on Meadow. Staff on Willow ward locked the patient’s en suite rooms which meant patients had to request staff to unlock them for access. and staff locking en suites on Willow. Managers told us that patients themselves had requested set snack times and to not have shoes on wards. Staff provided minutes of community meetings, however only records for two wards indicated patient agreement.
Advertisement
Hide AdAdvertisement
Hide AdManagers had not always ensured that there were the required numbers of staff on all shifts. Managers had not filled 13% of shifts between 1 and 31 March 2019. Managers had used bank and agency staff to cover 47% of shifts. Staff shortages sometimes resulted in staff cancelling escorted leave, appointments or ward activities. Staff on Fern, Maple and Willow wards told inspectors that the high use of bank and agency staff impacted on patient care as risk events increased due to inconsistencies in patient care.
Governance arrangements had not always identified that staff practices were sometimes in breach of the Mental Health Act Code of Practice. The provider had not addressed issues with restrictive practices and the environment previously raised by the CQC. Provider audits had failed to address the issues with restrictive practices. Managers did not always deal with risk issues appropriately or in a timely way. Although the provider had carried out work to rectify hazards, it was incomplete. The provider did not have a system to check that the maintenance team had completed required works satisfactorily.